Global Payment Integrity Software Market By Component (Software (On-Premises, Cloud-Based), Services), By Application (Claims Auditing, Fraud Detection, Payment Accuracy, Others), By End-User (Healthcare Payers, Government Agencies, TPAs, Others), By Regional Analysis, Global Trends and Opportunity, Future Outlook By 2025-2035
- Published date: Apr. 2026
- Report ID: 184307
- Number of Pages: 274
- Format:
-
keyboard_arrow_up
Quick Navigation
- Report Overview
- Top Market Takeaways
- Drivers Impact Analysis
- Restraints Impact Analysis
- By Component Analysis
- By Application Analysis
- By End-User Analysis
- Investor Type Impact Analysis
- Technology Enablement Analysis
- Key Challenges
- Emerging Trends
- Growth Factors
- Key Market Segments
- Regional Analysis
- Competitive Analysis
- Future Outlook
- Recent Developments
- Report Scope
Report Overview
The Global Payment Integrity Software Market generated USD 2.3 billion in 2025 and is predicted to register growth from USD 2.6 billion in 2026 to about USD 180.24 billion by 2035, recording a CAGR of 10.90% throughout the forecast span. In 2025, North America held a dominant market position, capturing more than a 40.3% share, holding USD 0.93 Billion revenue.
Top Market Takeaways
- Payment Integrity Software Market emphasizes software solutions focused on claims auditing for healthcare payers, with North America dominating due to rising healthcare costs and regulatory pressures for accurate reimbursements.
- Software holds 63.1% market share, providing AI-driven analytics for real-time payment validation, duplicate detection, and compliance automation across payer workflows.
- Claims auditing captures 37.8%, enabling prepayment and post-payment reviews to identify overpayments, coding errors, and fraud patterns in medical billing processes.
- Healthcare payers lead at 44.3%, using these tools for risk adjustment, utilization management, and recovery of improper payments to optimize financial operations.
- North America accounts for 40.3% globally, with the U.S. market valued at USD 0.84 billion and 8.7% CAGR, driven by Medicare/Medicaid scrutiny and private insurer efficiency demands.
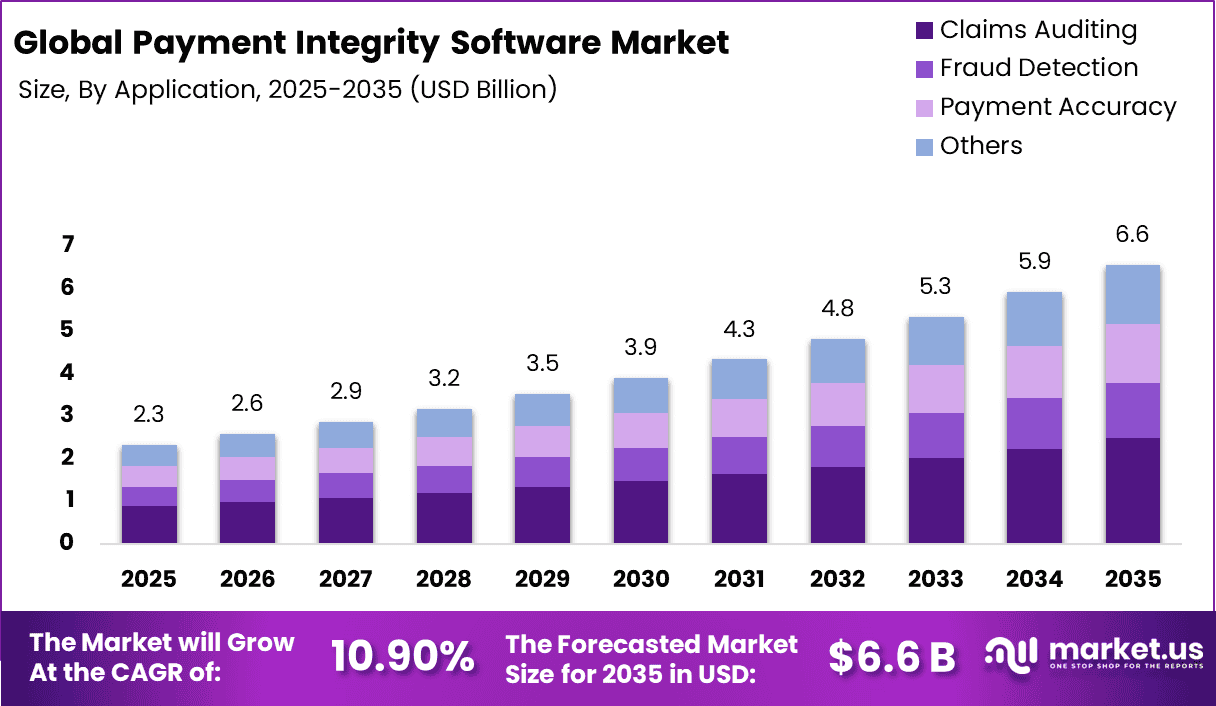
Payment integrity software is used to ensure that financial transactions are accurate, compliant, and free from errors or fraud. It is widely applied in sectors such as healthcare, insurance, and finance where large volumes of claims and payments are processed regularly.
The software reviews transactions before and after payment to identify issues such as duplicate payments, incorrect billing, or policy violations. As organizations handle increasing amounts of financial data, there is a growing need for systems that can improve accuracy and maintain control over payment processes.
One of the main driving factors is the rising concern around financial losses caused by billing errors and fraudulent activities. Organizations are under pressure to improve transparency and accountability in their payment systems. In addition, regulatory requirements are becoming more strict, which is encouraging companies to adopt tools that can support compliance and audit processes.
The growing use of digital payment systems and automated workflows is also increasing the need for solutions that can monitor transactions in real time. Advances in data analytics are further helping these systems detect patterns and identify irregularities more effectively.
Demand for payment integrity software is increasing as organizations look for ways to reduce financial leakage and improve operational efficiency. There is a strong preference for solutions that can integrate with existing systems and provide clear insights into transaction data. Users are also seeking tools that can automate reviews and reduce manual intervention, allowing teams to focus on higher value tasks.
The demand is particularly strong in environments where transaction volumes are high and accuracy is critical. As financial operations continue to become more complex, the need for reliable and intelligent payment validation solutions is expected to grow steadily.
Drivers Impact Analysis
Key Driver Impact on CAGR Forecast (~%) Geographic Relevance Impact Timeline Additional Insight Rising healthcare fraud and billing errors +3.4% North America, Europe Medium to long term Fraud detection drives software demand Increasing focus on cost containment in healthcare +3.1% Global Medium term Providers aim to reduce unnecessary expenses Growing adoption of data analytics in healthcare systems +2.8% Developed markets Medium to long term Analytics improves payment accuracy Regulatory pressure for transparency and compliance +2.6% North America, Europe Medium term Compliance needs boost adoption Expansion of health insurance coverage and claims volume +2.3% Global Medium to long term Higher claims require validation tools Restraints Impact Analysis
Key Restraint Impact on CAGR Forecast (~%) Geographic Relevance Impact Timeline Additional Insight High implementation and integration costs -2.7% Emerging markets Short to medium term Cost limits smaller provider adoption Complexity in integrating with legacy healthcare systems -2.3% Global Medium term Integration delays deployment Data privacy and security concerns -2.0% North America, Europe Medium to long term Sensitive data creates hesitation Limited awareness in developing healthcare systems -1.7% Developing regions Medium term Adoption remains slow Dependence on accurate and standardized data inputs -1.5% Global Long term Poor data quality affects outcomes By Component Analysis
The software segment accounted for 63.1% of the market share, reflecting its central role in identifying payment errors and improving financial accuracy within healthcare systems. This dominance is supported by the growing need for automated tools that can analyze large volumes of claims data and detect inconsistencies in billing and reimbursement processes. Software solutions help reduce manual effort and enhance transparency, which is essential for maintaining financial control.
Another factor driving this segment is the increasing complexity of healthcare payment systems. Advanced software platforms offer real-time analytics, rule-based validation, and predictive capabilities that improve decision-making. Their ability to integrate with existing systems and support continuous monitoring strengthens their adoption across healthcare organizations.
By Application Analysis
The claims auditing segment held 37.8% share, driven by the need to ensure accuracy and compliance in healthcare billing. Claims auditing helps identify overpayments, underpayments, and fraudulent activities, which can impact overall financial performance. Software tools streamline the auditing process by providing detailed insights and automated verification, making it more efficient and reliable.
In addition, the growing focus on cost control and regulatory compliance has increased the importance of effective auditing processes. Organizations are adopting advanced solutions to improve accuracy and reduce financial risks. This has strengthened the role of claims auditing within the payment integrity software market.
By End-User Analysis
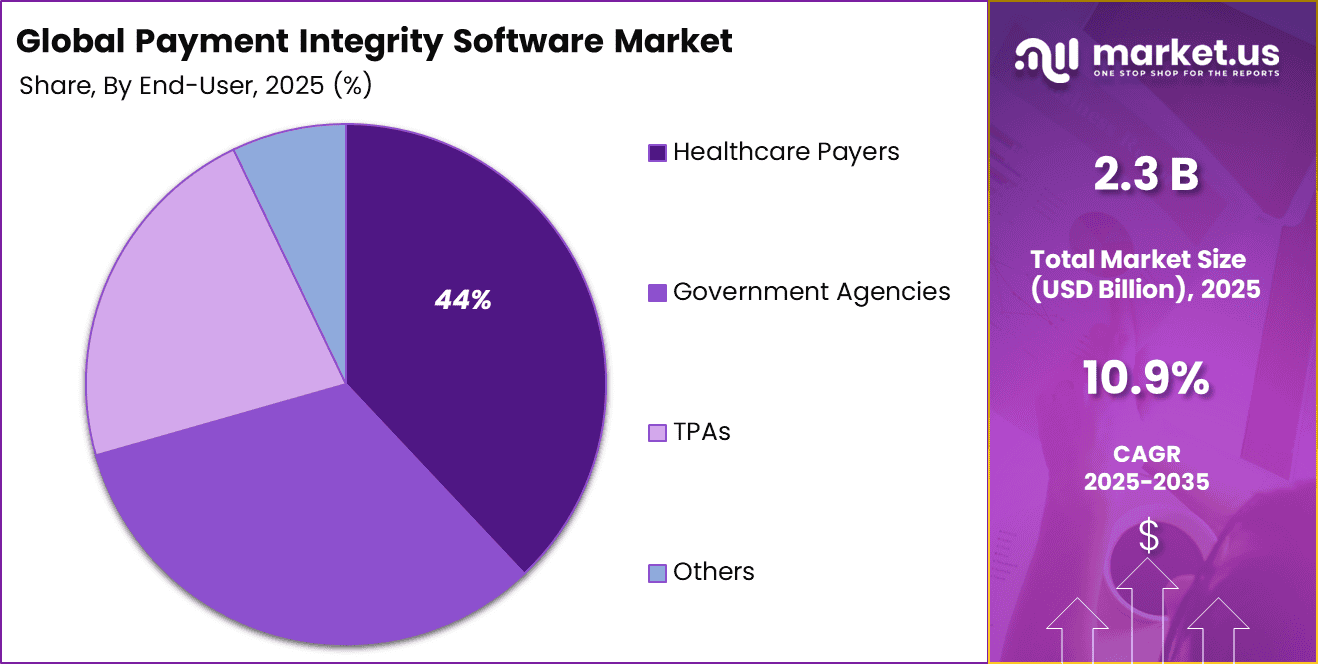
The healthcare payers segment captured 44% of the market, driven by their responsibility to manage large volumes of claims and ensure accurate reimbursements. Payers rely on payment integrity software to detect errors, prevent fraud, and optimize financial operations. These tools help improve efficiency and support better management of healthcare spending.
Furthermore, increasing pressure to control costs and maintain compliance with regulatory standards has encouraged payers to invest in advanced solutions. Payment integrity software enables better oversight of payment processes and reduces the likelihood of financial losses. This has made it an essential component for healthcare payers aiming to enhance operational efficiency.
Investor Type Impact Analysis
Investor Type Growth Sensitivity Risk Exposure Geographic Focus Investment Outlook Venture capital firms High High US, Europe Investing in healthcare analytics startups Private equity firms Moderate to high Moderate North America and Europe Scaling payment integrity solution providers Corporate investors High Moderate Global Strategic investments in healthcare IT systems Institutional investors Moderate Low to moderate Developed markets Prefer stable healthcare technology firms Government and public funding bodies Moderate to high Low US, EU Supporting healthcare transparency initiatives Technology Enablement Analysis
Technology Impact on CAGR Forecast (~%) Geographic Relevance Impact Timeline Additional Insight AI and machine learning for fraud detection +3.6% US, Europe Medium to long term Enhances detection accuracy Cloud-based payment integrity platforms +3.2% Global Short to medium term Enables scalable deployment Predictive analytics for claims validation +2.9% Developed markets Medium term Improves decision-making Integration with electronic health records (EHR) +2.6% Global Medium to long term Streamlines data access Automation of claims auditing processes +2.3% Global Medium term Reduces manual errors and workload Key Challenges
- High implementation cost makes it difficult for small healthcare providers to adopt.
- Complex integration with existing billing and claims systems.
- Data accuracy issues due to incomplete or inconsistent healthcare records.
- Strict regulatory requirements increase compliance burden.
- Limited skilled professionals to manage and analyze payment data.
- Resistance to change from traditional manual processes.
- Data privacy and security concerns with sensitive patient information.
- Difficulty in handling large volumes of claims data.
- Frequent updates needed to keep up with changing policies and rules.
- Dependence on advanced analytics tools for accurate results.
Emerging Trends
The payment integrity software market is evolving toward more proactive and intelligence driven systems that focus on preventing errors before they occur rather than identifying them after processing. One key emerging trend is the use of advanced analytics and AI to review claims and transactions in real time, helping detect inconsistencies, duplicate entries, and incorrect billing patterns early in the process.
Another important trend is the integration of payment integrity tools with broader healthcare management systems, allowing seamless data exchange and better coordination across workflows. There is also growing adoption of automated audit and validation features that reduce manual review efforts and improve accuracy. In addition, predictive modeling is being used to flag high risk claims based on historical patterns, enabling more targeted intervention. The shift toward cloud based platforms is further supporting scalability and remote access, making these solutions easier to deploy and manage across large healthcare networks.
Growth Factors
The growth of this market is driven by the increasing need to control rising healthcare costs and improve financial transparency. Organizations are focusing on reducing payment errors, fraud, and inefficiencies, which is encouraging the adoption of advanced integrity solutions. The growing complexity of healthcare billing systems and coding structures is also creating demand for software that can ensure compliance and accuracy.
Another major factor is the rising volume of claims and transactions, which makes manual verification difficult and time consuming. Healthcare providers and payers are also under pressure to improve operational efficiency and maintain regulatory compliance, further supporting the use of automated tools. Additionally, the shift toward value based care models is pushing organizations to ensure that payments are aligned with actual services delivered, strengthening the role of payment integrity software in maintaining trust and accountability within the system.
Key Market Segments
By Component
- Software
- On-Premises
- Cloud-Based
- Services
By Application
- Claims Auditing
- Fraud Detection
- Payment Accuracy
- Others
By End-User
- Healthcare Payers
- Government Agencies
- TPAs
- Others
Regional Analysis
North America accounted for 40.3% of the Payment Integrity Software market, supported by the strong presence of advanced healthcare systems and increasing focus on cost control and fraud prevention. The region is witnessing growing adoption of digital tools to identify billing errors, detect fraudulent claims, and improve payment accuracy across healthcare providers and payers.
Organizations are placing higher emphasis on transparency and compliance, which is encouraging the use of automated audit and analytics solutions. In addition, the complexity of healthcare reimbursement processes is driving demand for software that can streamline claim reviews and ensure proper payment practices.
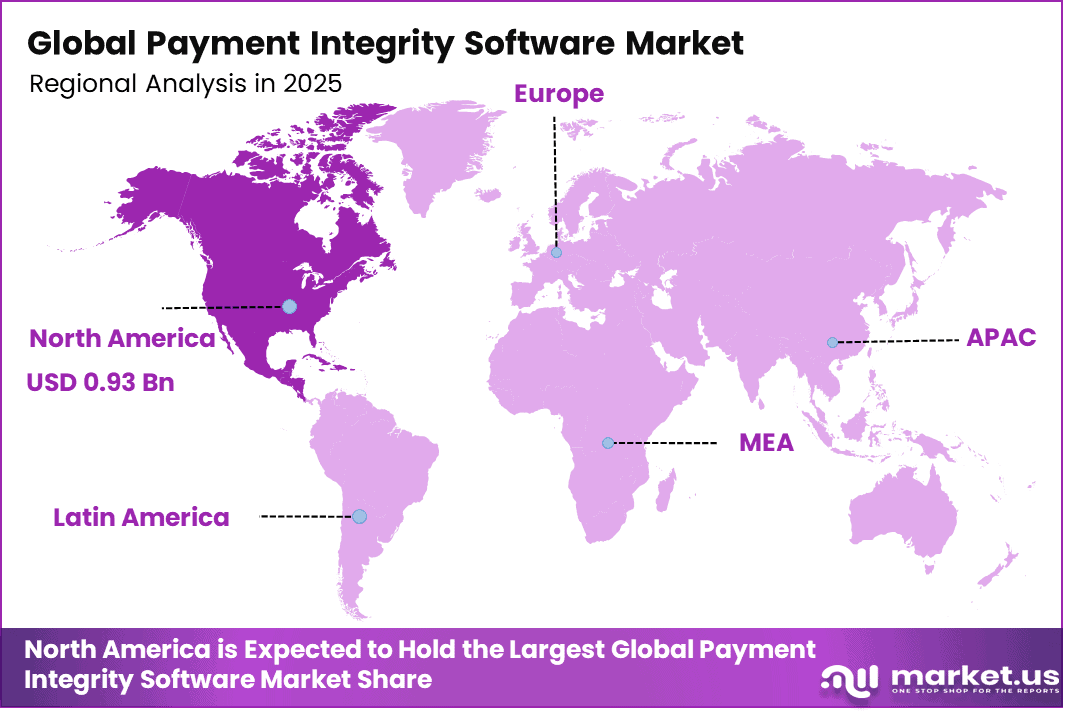
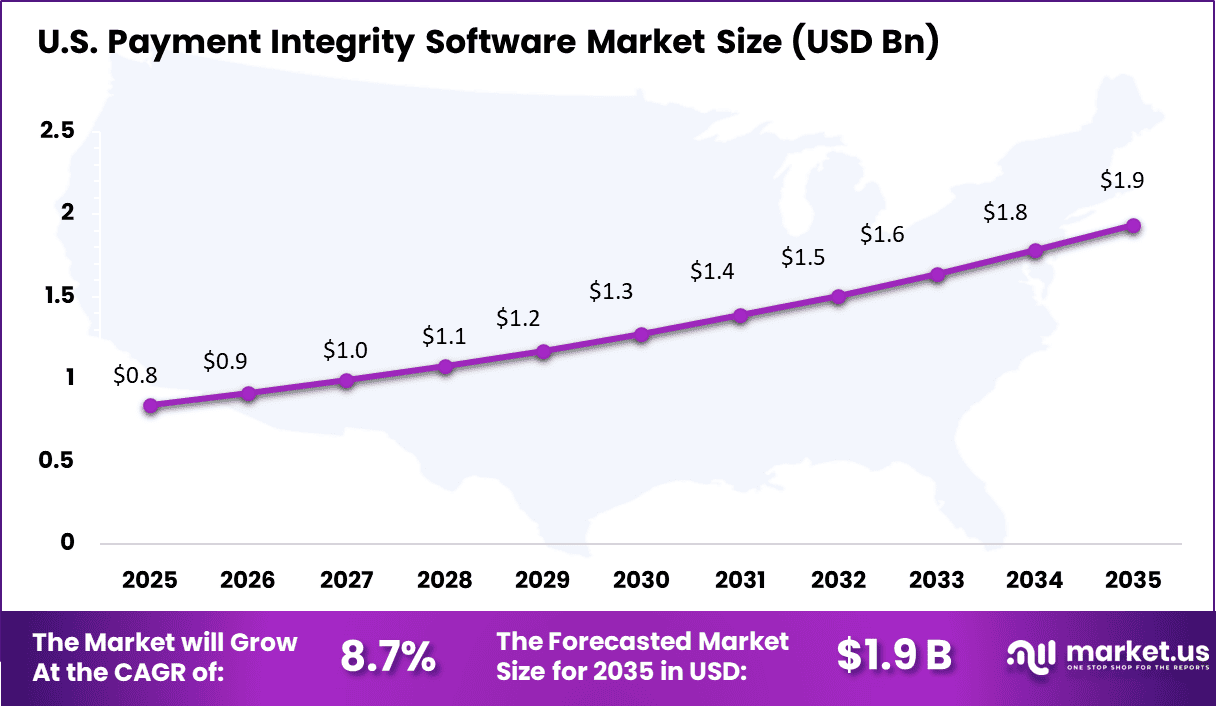
The U.S. market reached USD 0.84 Billion and is projected to grow at a CAGR of 8.7%, driven by rising healthcare expenditure and increasing need to manage financial leakages. Healthcare payers and providers are adopting payment integrity solutions to enhance operational efficiency and reduce losses from incorrect claims.
The growing use of data analytics and automation is improving the ability to identify anomalies and ensure compliance with regulatory standards. As the healthcare system continues to evolve and become more data-driven, the demand for payment integrity software in the US is expected to maintain steady growth over the coming years.
Key Regions and Countries
- North America
- US
- Canada
- Europe
- Germany
- France
- The UK
- Spain
- Italy
- Russia
- Netherlands
- Rest of Europe
- Asia Pacific
- China
- Japan
- South Korea
- India
- Australia
- Singapore
- Thailand
- Vietnam
- Rest of APAC
- Latin America
- Brazil
- Mexico
- Rest of Latin America
- Middle East & Africa
- South Africa
- Saudi Arabia
- UAE
- Rest of MEA
Competitive Analysis
The competitive landscape of the Payment Integrity Software Market is led by a mix of healthcare analytics providers, consulting firms, and technology companies. Companies such as Cotiviti Holdings, LLC, Optum, Inc., Change Healthcare, Inc., and Truven Health Analytics (an IBM Company) focus on advanced payment accuracy, claims auditing, and fraud detection solutions.
These players use data analytics, automation, and rule-based systems to help healthcare payers reduce billing errors and control costs. Their strong domain expertise and large healthcare datasets support their leadership in the market.
At the same time, companies such as EXL Service, Cognizant Technology Solutions, Mphasis Ltd., Firstsource Solutions Limited, and Infogain Corporation provide outsourced services and analytics support to enhance payment integrity operations.
Firms like SAS Institute Inc., Verisk Analytics, Inc., Clarify Health Solutions, HealthEdge Software, Inc., MedData, Inc., Mitchell International, Inc., Teladoc Health, Inc., and Equifax Inc. focus on data-driven insights, risk management, and workflow optimization. Competition in this market is driven by accuracy of analytics, ease of integration with healthcare systems, and the ability to detect fraud and errors in real time.
Top Key Players in the Market
- Cotiviti Holdings, LLC
- Optum, Inc.
- HCG Health Software Solutions
- Change Healthcare, Inc.
- Mitchell International, Inc.
- EXL Service
- Truven Health Analytics (an IBM Company)
- MedData, Inc.
- Teladoc Health, Inc.
- Equifax Inc.
- SAS Institute Inc.
- Verisk Analytics, Inc.
- Clarify Health Solutions
- Cognizant Technology Solutions
- HealthEdge Software, Inc.
- Mphasis Ltd.
- Firstsource Solutions Limited
- Infogain Corporation
- Other Key Players
Future Outlook
The future outlook for the Payment Integrity Software Market looks strong as healthcare organizations continue to focus on reducing billing errors, fraud, and unnecessary costs. The market is expected to grow with the increasing need for accurate claims processing and better financial control. More providers and payers are anticipated to adopt advanced software to review payments and improve transparency. In the coming years, the use of AI and data analytics is expected to make these solutions more effective in detecting issues early, helping organizations save costs and improve overall efficiency.
Recent Developments
- February, 2026 – Cotiviti launches phased 2026 regulatory prep toolkit scanning telehealth billing spikes. AI monitors skin substitute claims under new incident-to rules while provider pattern analysis flags waste. Phased approach builds proactive risk mitigation saving 15% on audits.
- January, 2026 – Optum expands pre/post-payment suite with AI-driven COB matching across 50M lives. Real-time underpayment recovery boosts cash flow 12% while service gaps prompt support upgrades. Broadest portfolio serves Medicare Advantage leaders.
Report Scope
Report Features Description Market Value (2025) USD 2.3 Billion Forecast Revenue (2035) USD 6.6 Billion CAGR(2025-2035) 10.90% Base Year for Estimation 2024 Historic Period 2020-2024 Forecast Period 2025-2035 Report Coverage Revenue forecast, AI impact on Market trends, Share Insights, Company ranking, competitive landscape, Recent Developments, Market Dynamics and Emerging Trends Segments Covered By Component (Software (On-Premises, Cloud-Based), Services), By Application (Claims Auditing, Fraud Detection, Payment Accuracy, Others), By End-User (Healthcare Payers, Government Agencies, TPAs, Others) Regional Analysis North America – US, Canada; Europe – Germany, France, The UK, Spain, Italy, Russia, Netherlands, Rest of Europe; Asia Pacific – China, Japan, South Korea, India, New Zealand, Singapore, Thailand, Vietnam, Rest of Latin America; Latin America – Brazil, Mexico, Rest of Latin America; Middle East & Africa – South Africa, Saudi Arabia, UAE, Rest of MEA Competitive Landscape Cotiviti Holdings, LLC, Optum, Inc., HCG Health Software Solutions, Change Healthcare, Inc., Mitchell International, Inc., EXL Service, Truven Health Analytics (an IBM Company), MedData, Inc., Teladoc Health, Inc., Equifax Inc., SAS Institute Inc., Verisk Analytics, Inc., Clarify Health Solutions, Cognizant Technology Solutions, HealthEdge Software, Inc., Mphasis Ltd., Firstsource Solutions Limited, Infogain Corporation, Other Key Players Customization Scope Customization for segments, region/country-level will be provided. Moreover, additional customization can be done based on the requirements. Purchase Options We have three license to opt for: Single User License, Multi-User License (Up to 5 Users), Corporate Use License (Unlimited User and Printable PDF)  Payment Integrity Software MarketPublished date: Apr. 2026add_shopping_cartBuy Now get_appDownload Sample
Payment Integrity Software MarketPublished date: Apr. 2026add_shopping_cartBuy Now get_appDownload Sample -
-
- Cotiviti Holdings, LLC
- Optum, Inc.
- HCG Health Software Solutions
- Change Healthcare, Inc.
- Mitchell International, Inc.
- EXL Service
- Truven Health Analytics (an IBM Company)
- MedData, Inc.
- Teladoc Health, Inc.
- Equifax Inc.
- SAS Institute Inc.
- Verisk Analytics, Inc.
- Clarify Health Solutions
- Cognizant Technology Solutions
- HealthEdge Software, Inc.
- Mphasis Ltd.
- Firstsource Solutions Limited
- Infogain Corporation
- Other Key Players













